Lake Nona Medical Arts’ Dr. Richard Gayles: Phantom Limb Pain Affects Majority of Amputees
By By Dr. Richard Gayles // August 16, 2016
DIFFICULT TO TREAT AND ON THE RISE

If you or a family member have suffered with PLP and would like to discuss treatment, please contact Dr. Richard Gayles, founder and director of Lake Nona Medical Arts, at 407-412-5030.
LAKE NONA, FLORIDA – Phantom limb pain (PLP), a devastating condition that may follow the loss of a limb from any cause, is pain perceived to come from a limb that is no longer present.
PLP is different from phantom sensations, which are non-painful perceptions that the limb is still present even though that part of the body no longer exists. PLP may also be confused with pain at the site of the amputation, which is called stump pain.

Between 42 and 79 percent of amputees report some phantom phenomenon, and the majority of these are painful. The most common sensations include tingling, throbbing, piercing and pins and needles.
The onset of phantom sensation and PLP may occur immediately after amputation or be delayed weeks, months or even years following the surgery, with two peak periods of PLP, at one month and one year after amputation.
Fortunately, in most cases, the intensity of these unpleasant sensations declines with time.
POORLY UNDERSTOOD, DIFFICULT TO TREAT – AND ON THE RISE
A Civil War surgeon, Silas Weir Mitchell, coined the term phantom limb, which commonly followed battlefield amputations. Today PLP continues to remain a poorly understood condition, which is difficult to treat.

There are currently 1.5 million amputees in the Unites States, and the number is expected grow to about 3.6 million by 2050. Common causes of limb loss include compromised blood flow to the limbs called peripheral vascular insufficiency, trauma, cancer and congenital limb deficiency.
PLP is most common after loss of a limb, but may occur from the loss of any organ or body part, and has been seen following surgery involving removal of organs such as breast, bowels, bladder, penis and eyes – as well as post tooth extraction.
PLP MAY ORIGINATE AT THE STUMP, SPINAL CORD OR BRAIN
Risk factors for PLP include female gender, upper extremity amputation, presence of pre-amputation pain, stump pain and poorly fitting artificial limbs. Anxiety, depression or other emotional triggers do not cause PLP, but are believed to contribute to its exacerbation and persistence.

Mechanisms or causes of PLP are not well understood, but can be roughly divided in peripheral and central causes. Peripheral causes are located in the residual part of the amputated limb and central causes are located in the brain and spinal cord.
Peripheral mechanisms include persistent pain in the residual limb or stump from any cause, including a poorly fitting prosthesis. A frequent peripheral PLP cause is the abnormal excitability in a neuroma, which is a tangled growth of nerve fibers at the cut end of a nerve within the stump.
“A neuroma resembles a mushroom cap, is extremely irritable, sensitive, and painful, and can be thought of as the cut end of a high voltage power line which seems to spontaneously spark and hiss with electrical activity.”
A neuroma resembles a mushroom cap, is extremely irritable, sensitive, and painful, and can be thought of as the cut end of a high voltage power line which seems to spontaneously spark and hiss with electrical activity. The abnormal electrical activity of the neuroma travels back along the nerve into the spinal cord, which is bombarded by this intense input and in turn causes abnormal excitation, sensitivity, and reactivity of the spinal cord.
Central mechanisms are even less well understood. Loss of sensation (sensory input) following amputation into the spinal cord, can lead to new and abnormal connections between nerves. Nerves from intact areas tend to sprout or grow into areas where there is sensory loss following amputations.
The abnormal new connections and circuits are thought to be one of the major causes of PLP. Similar changes are thought to occur in the brain where new and abnormal connections are made, distorting highly ordered structure, activity and organization.
PLP PRESENTS THERAPEUTIC CHALLENGE
Because effectively treating PLP has been so challenging, many treatment modalities have been tried.
 Preemptive analgesia is used in some centers to help prevent PLP. Continuous epidurals are placed 48 hours prior to surgery, providing complete relief of limb pain that is often present before many amputations.
Preemptive analgesia is used in some centers to help prevent PLP. Continuous epidurals are placed 48 hours prior to surgery, providing complete relief of limb pain that is often present before many amputations.
The epidural is continued through the operation to 48 hours post procedure, suppressing activity within the spinal cord, and thus helping to prevent PLP.
Medications have been used with some success to treat PLP, and include narcotic pain medication, anti-depressants, NSAIDS, anti-convulsants (Neurontin or Lyrica) and tramadol. These may be taken either alone or in combination.
In addition to preemptive analgesia and medications, various other types of therapies such as acupuncture, ultrasound, massage, TENS units, physiotherapy and prosthesis training have been used.
“In addition to preemptive analgesia and medications, various other types of therapies such as acupuncture, ultrasound, massage, TENS units, physiotherapy and prosthesis training have been used.”
Biofeedback and cognitive behavioral pain management are therapeutic techniques that may help build coping skills to deal with the emotional consequences of PLP.
Invasive and surgical procedures to reduce phantom limb pain from stump neuromas have also been effective. Destruction of the neuroma with radiofrequency ablation (cauterization) can stop its hyperactivity. Surgical clipping of the neuroma, in which the abnormally active neuroma tip is cut off and the cut end is buried in healthy tissue, can also be effective in some cases. By ablating or removing the neuroma the nerve is not abnormally and spontaneously active.
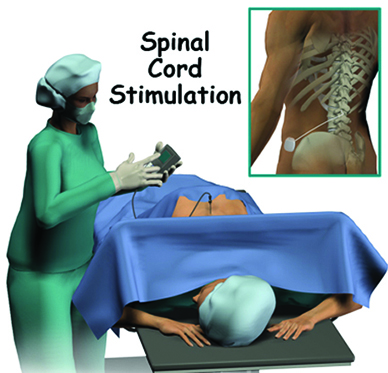
SPINAL CORD STIMULATION IS EFFECTIVE FOR STUMP, PLP PAIN
If the above measures fail, spinal cord stimulation (SCS) may be an effective tool for the control of both stump pain and phantom limb pain.

SCS is a reversible technique that involves placing a tiny wire or electrode in the spine.
The electrode produces an electrical current that blocks pain signals from the stump and PLP from traveling to the brain, and the patient becomes much less aware of the pain.
SCS has been used extensively for these conditions in Europe and the US.
If you or a family member have suffered with PLP and would like to discuss treatment, please contact Dr. Richard Gayles at 407-412-5030.
ABOUT THE AUTHOR
Dr. Richard Gayles is the founder and director of Lake Nona Medical Arts and brings a wealth of training and experience to pain management. He received a Bachelor of Science in Psychobiology from the University of Michigan in 1987 and his Doctor of Medicine in 1991 at the University of Michigan’s School of Medicine. After graduation, he completed a residency and Pediatric Anesthesia Fellowship in the Department of Anesthesiology and Critical Care Medicine at Johns Hopkins Hospital in Maryland.

Dr. Gayles obtained further clinical experience in anesthesiology at St. Bartholomew’s Hospital in London, England. He completed a Chronic Pain Fellowship at the Cleveland Clinic Foundation in Ohio, where he was awarded the “Fellow of the Year Award” in June of 1997.
In addition to his clinical experience, Dr. Gayles has participated in research over the past 14 years, both here at home and abroad. Dr. Gayles is Board Certified by the American Board of Anesthesiology and a Diplomat of the American Academy of Pain Management. He is also certified by the American Board of Pain Medicine, National Board of Medical Examiners and by the American Heart Association in Basic and Advanced Cardiac Life Support. Dr. Gayles holds the Following Special Affiliations: Member of Coast Guard Auxiliary and FAA (an Aero Medical Examiner) ANGEL Flight.
To make an appointment with Dr. Gayles, call 407-412-5030, and for more information, log on to LakeNonaMedicalArts.com












