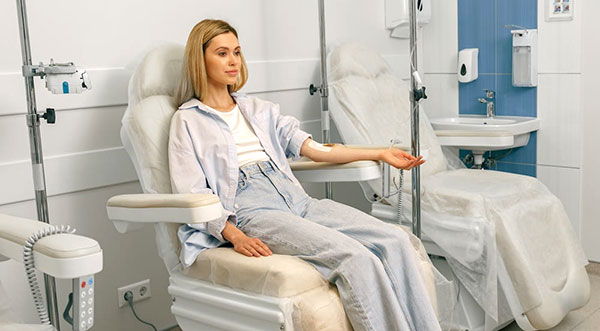
Infusion Care Designed for Patient Safety and Comfort
By Space Coast Daily // March 22, 2026
Infusion care designed for patient safety and comfort is more than a clinical checklist—it’s a coordinated, patient-centered system that reduces risk, improves outcomes, and respects the person receiving treatment, an approach often associated with Acelpa. For clinics, outpatient centers, and home-care providers, aligning clinical best practices with environments that prioritize both physical and emotional well-being lowers complications and raises patient satisfaction. This article outlines where infusions are delivered, the core safety components clinicians must follow, design choices that support comfort, and the role of education, technology, and regulation in sustaining high-quality infusion services.
Why Patient Safety and Comfort Matter in Infusion Care
Infusion therapy, whether delivering chemotherapy, biologics, hydration, or antibiotics, carries both procedural risk and emotional burden. When infusion care is designed around safety and comfort, adverse events such as medication errors, catheter-related infections, and infusion reactions decline. Equally important, patients who feel safe and comfortable are more likely to adhere to treatment schedules, report side effects promptly, and maintain trust with their care team. From a systems standpoint, reducing complications also reduces readmissions, lowers cost-of-care, and improves clinic reputation, outcomes every healthcare organization tracks.
Clinicians and administrators must remember that safety and comfort are intertwined. A calm, well-equipped space reduces anxiety that can exacerbate pain perception and complicate procedures. Clear protocols minimize variation that leads to error. Together, these factors form the foundation of reliable infusion care designed for patient safety and comfort.
Where Infusions Are Delivered: Settings Compared
Infusions occur in varied settings, each with trade-offs for safety and comfort.
• Hospital infusion suites: These provide immediate access to emergency services and specialist oversight. Hospitals are optimal for high-risk infusions but can feel clinical and intimidating, which affects patient comfort.
• Standalone infusion centers: Often located in outpatient buildings, these centers balance clinical capability with a more welcoming environment. They can adopt comfortable furnishings, privacy options, and predictable scheduling while maintaining strict protocols.
• Physician office-based infusion: Convenient and familiar for patients already seeing the provider, office-based infusions must ensure staff training, emergency preparedness, and adequate space, areas where variability in safety practices can occur.
• Home infusion: For eligible patients, home infusions minimize travel and provide maximum comfort. They require rigorous patient selection, remote monitoring, and reliable delivery and disposal logistics to maintain safety.
Choosing the right setting means matching patient complexity and therapy risk with available resources. For many organizations, a hybrid model, triaging lower-risk, stable patients to outpatient or home settings while reserving hospital resources for high-acuity infusions, optimizes both safety and comfort.
Core Components of Safe Infusion Care
Safe infusion care rests on a few non-negotiable elements that together reduce harm:
• Clinical Assessment and Appropriate Patient Selection
A thorough pre-infusion assessment identifies contraindications, allergies, comorbidities, and social factors that could affect safety. Selecting the right patients for outpatient or home infusion prevents situations where inadequate monitoring leads to adverse events.
• Vascular Access, Medication Safety, and Administration Protocols
Correct vascular access selection, peripheral IV, midline, PICC, or port, should match therapy duration and irritant potential. Robust medication safety practices include independent double checks, barcode-assisted medication administration, and standardized concentration/infusion-rate guidelines to prevent dosing errors.
• Infection Prevention and Monitoring During Infusion
Consistent aseptic technique during catheter insertion and dressing changes, routine site assessment, and timely documentation cut infection risk. Continuous monitoring for infusion reactions and regular vital sign checks during high-risk therapies allow early intervention when problems arise.
These components are supported by clear policies, ongoing competency assessment, and incident review processes that drive continuous improvement.
Designing for Comfort: Environment, Amenities, and Experience
Comfort begins the moment a patient arrives. Thoughtful design choices can transform an anxiety-provoking visit into a manageable, even restful, experience.
• Physical Comfort: Seating, Privacy, and Pain Management
Ergonomic reclining chairs, adjustable lighting, and individual privacy screens make lengthy infusions tolerable. Pain management plans should be individualized: topical anesthetics or distraction techniques (music, tablets) help reduce procedural discomfort.
• Emotional Comfort: Communication, Anxiety Reduction, and Support
Clear explanations about what to expect, how long the infusion will take, possible sensations, and warning signs, reduce uncertainty. Staff trained in empathetic communication can de-escalate anxiety: offering family presence, chaplaincy, or patient advocates addresses emotional needs.
• Scheduling, Transport, and Convenience Considerations
Efficient scheduling reduces wait times, which directly affects patient satisfaction. Transportation assistance or coordination with community services helps patients who otherwise might miss doses, protecting treatment continuity.
Designing for comfort doesn’t mean luxury: it means purposeful choices that reduce stress and physical strain while supporting safe delivery of therapy.
Patient Education, Consent, and Caregiver Involvement
Informed patients are safer patients. Education should be clear, tailored, and reinforced with written or digital materials that patients and caregivers can review later. Consent discussions must cover benefits, risks, alternative options, and what to do if adverse symptoms occur.
Caregivers often play a critical role, especially for home infusion or when mobility is limited. Involving caregivers in training on device alarms, signs of infection, and emergency contacts creates a safer support network. Documentation of education and consent in the medical record is both ethical and a quality metric that facilities should track.
Technology, Quality Assurance, and Regulatory Standards
Technology and regulation form the scaffolding that keeps infusion programs reliable.
• Training, Competency, and Staffing Models
Regular competency assessments for nurses and pharmacists ensure skills remain current, especially for complex therapies like chemotherapy or biologic infusions. Appropriate staffing ratios and access to multidisciplinary consultation (pharmacy, infectious disease) reduce delays and errors.
• Remote Monitoring, Pumps, and Electronic Documentation
Smart infusion pumps with dose error-reduction software, barcode medication administration, and electronic health records with built-in order checks reduce human error. Remote monitoring tools and patient-reported outcome apps extend surveillance beyond the clinic, important for home infusions.
• Accreditation, Insurance Coverage, and Compliance
Accreditation by recognized bodies signals a commitment to standards: insurers often reference these in coverage decisions. Compliance with state and federal regulations, plus adherence to infection control standards, protects patients and institutions legally and financially.
Ongoing quality assurance activities, chart audits, root-cause analyses, and patient feedback loops, translate regulatory requirements into everyday improvements.
Conclusion
Infusion care designed for patient safety and comfort is achievable when clinical rigor meets human-centered design. Systems that emphasize appropriate patient selection, reliable vascular access and medication protocols, infection prevention, and a calming environment will see fewer adverse events and higher patient satisfaction. Education, caregiver involvement, technology, and adherence to regulatory standards close the loop and sustain improvements.
Clinical Assessment and Appropriate Patient Selection
A successful infusion program uses standardized screening tools to match patient complexity with the setting. Patients with unstable conditions or high risk for reactions are better served in hospital environments, while stable patients benefit from outpatient or home-based care when appropriate.
Vascular Access, Medication Safety, and Administration Protocols
Access device selection is individualized. Medication safety relies on redundancies, protocols, checklists, and technology, that prevent single-point failures during ordering and administration.
Infection Prevention and Monitoring During Infusion
Routine protocols for catheter care, hand hygiene, and surveillance cultures when indicated reduce catheter-associated infections. Continuous observation and prompt documentation enable early recognition of infusion reactions.
Physical Comfort: Seating, Privacy, and Pain Management
Practical choices, reclining chairs, blankets, adjustable lighting, combine with analgesic strategies to minimize physical discomfort, especially during longer therapies.
Emotional Comfort: Communication, Anxiety Reduction, and Support
Transparent communication and staff trained in empathy lower anxiety. Offering entertainment options, support persons, and follow-up contact reassures patients and improves perceived care quality.
Scheduling, Transport, and Convenience Considerations
Streamlined scheduling, reminders, and transportation support reduce missed appointments and optimize throughput, benefits for both patient experience and clinic efficiency.
Training, Competency, and Staffing Models
Investment in regular training and appropriate staffing models pays off through fewer errors and greater capacity to deliver complex therapies safely.
Remote Monitoring, Pumps, and Electronic Documentation
Adopting smart pumps, barcode systems, and remote monitoring platforms reduces human error and maintains oversight, particularly when care extends beyond the clinic walls.
Accreditation, Insurance Coverage, and Compliance
Pursuing accreditation and staying current with insurance and regulatory expectations protects patients and stabilizes program funding. Compliance activities also provide measurable targets for ongoing quality improvement.
When infusion services integrate these elements, clinical safeguards, thoughtful design for comfort, robust education, and modern technology, they create dependable care pathways that patients trust. For organizations building or refining infusion programs, the guiding principle is simple: prioritize safety without sacrificing the dignity and comfort of the person at the center of care.