SPACE COAST DAILY HEALTH SPOTLIGHT: The ‘Art’ of Diabetes Control
By Myla Ross, Pharm D. // June 7, 2017
diligence, discipline, understanding of the disease are essential

BREVARD COUNTY, FLORIDA — Most people know that diabetes is a disease involving sugar and that some people are born with it (type 1 diabetes) and others develop it later in life, perhaps after many years of not watching what they eat and maybe having too much sugar in their diet (type 2 diabetes).
We also know that insulin plays a big part in the treatment of this disease. We’ve seen diabetics who have a pouch with insulin vials and needles, or friends and family members with their glucose monitors or insulin injector pens.
However, whether you’ve been a diabetic for the last 15 years or you’re still having a hard time understanding how having a disease that gives you high blood sugar puts you at risk for having low blood sugar, it’s important to understand the basics of diabetes, how it happens and what insulin does to help treat this condition.
Insulin, What Is It?
If you drive up to Fort Christmas Historical Park (about 25 minutes southwest of Titusville), you will find a display showcasing insulin bottles that belonged to Emmett Tanner. Mr. Tanner was the first person in Orange County to receive insulin injections in 1927.
Fast-forward to today and insulin is a widely used medication that becomes the focus of treatment for many diabetic patients. So what is this liquid we inject into ourselves, and what have we learned about it since we started using it over a century ago?
Insulin is a hormone made in the pancreas. When food is ingested containing carbohydrates (starches, dairy, and fruit) it is converted into sugar, which is dumped into the blood stream. Once your blood sugar levels start to increase, the pancreas kicks into action to make and release insulin, which acts as the “usher” to direct the sugar where to go.

If you are doing work and need energy immediately, the insulin drives the sugar into muscle cells so it can be used as fuel for that working cell. If there is no immediate need of energy from sugar because you are not currently working or you have more sugar than you need (you are relaxing on the couch and eating an apple), then the insulin moves the sugar into storage in the liver to wait for a time when it may be needed later (you go for a jog 2 hours later and now your cells need some extra energy).
Diabetes, What’s Broken?
Although they are both called diabetes, the two main types of diabetes are actually very different.
Type 1 diabetes is actually a kind of autoimmune disorder where the body attacks and destroys its own cells. Type 1 diabetics are younger and typically have a normal to slim body build when they are diagnosed. In this type of diabetes, specific pancreatic cells called beta cells, which normally make insulin and release it into the bloodstream, come under attack. Resulting in insulin deficiency.

Type 2 diabetics are usually a little older and often overweight. In fact, obesity is a primary risk factor for developing type 2 diabetes. In this type of diabetes the pancreas is still making some insulin, but production is insufficient, the release of insulin that is produced is diminished, and the body just doesn’t listen to what the insulin is telling it to do and becomes “resistant” to its commands.
This is why type 2 diabetes is often described as “impaired insulin secretion” and “insulin resistance.” To make matters worse, the liver (where the body makes and stores sugar) often sends extra sugar into the bloodstream resulting in elevated sugar in the blood that literally has no place to go since the body has stopped listening to the insulin that normally tells it to either go into the muscle cells or go into storage.
Myths About Diabetes and Insulin
Poor self-control and eating too much sugar is the reason people get diabetes. This is not the whole story. The inability to make and appropriately use insulin is the cause of diabetes. However, it is true that eating too much sugar can make it harder to control diabetes.
If you’ve ever wondered why you’re having such a hard time kicking the sugar habit, don’t feel bad, it’s not just you. In our hunter gatherer days, the sweet taste of carbohydrate rich food served a very important purpose. The taste of sweet gave us two vital pieces of information about the food we were eating: number one, it likely wasn’t poisonous and number two, it was full of sugar that could be easily used or stored.

Both of these messages translated to: eat as much of this as possible! Our ancestors with the strongest sweet tooth generally got more of the carbohydrate rich foods that allowed them to store more energy and keep them alive when food was scarce.
Thus, our desire to order the piece of cheesecake at the Italian restaurant after we’ve just filled up on pasta still drives us to make decisions that we know are probably not good for us in the long term. The good news is, the more we cut sugar out of our diets, the easier it is to keep it out.
There’s also a myth that people with type 1 diabetes cannot qualify for life insurance coverage. That’s simply not the case says Matt Schmidt of Diabetes Life Solutions.
Insurance companies have evolved, and have made lots of positive changes to their underwriting guidelines that have benefited the diabetes community. As an example, type 1 diabetes life insurance rates are at all-time lows in term of rates and premiums.
Being put on insulin means I’ve failed. As much as some people would like to avoid using insulin, for many people it is unavoidable no matter how well they manage their diabetes. In fact, many diabetes treatment specialists argue that insulin is the ideal treatment and prefer it over pills for their patients.
For type 1 diabetes insulin has to be taken because the body loses the ability to make it. For type 2 diabetes it is possible to treat the disorder with pills at first, but most people will eventually need to use insulin. This is because as time goes by, body changes and what used to work to keep blood sugar controlled in the past may no long be enough.
Insulin will make me gain a lot of weight. Weight gain is possible after starting insulin, but this is because sugar is being appropriately utilized under the effect of the therapeutic insulin. Along with diligent use of medications, eating a healthy diet and staying physically active are important elements of controlling diabetes and protecting against the ravishes of diabetic complications.

Insulin injections hurt. It can be scary being told you will have to use a needle to inject medication into your skin, but what you may not know, is that the needle is very small and there is very little to no pain involved.
All the patients I’ve met that were afraid to use insulin have been relieved by the reality of the situation once they got started. The fact is, a sharp clawed kitten or stinging bee can cause a lot more discomfort than an insulin needle and the insulin will help you to stay healthy and avoid the long term complications of high blood sugar that can be much more painful like nerve pain.
If insulin injections do cause pain, there may be something wrong with the way it is being injected, something as simple as not pressing so hard could be the fix that gives you a pain free injection. It’s also important to use a fresh needle for each injection and rotate the injection sites.
The Long and Short Of It—Types Of Insulin
In general, the two main types of insulin are long acting and short acting. Long acting insulin is usually taken at the same time every day to help keep blood sugar steady over long periods of time (over an entire day or half a day). Short acting insulin is used when a meal is ingested to help manage the spike in sugar resulting from the food.
Benefits Of Treatment
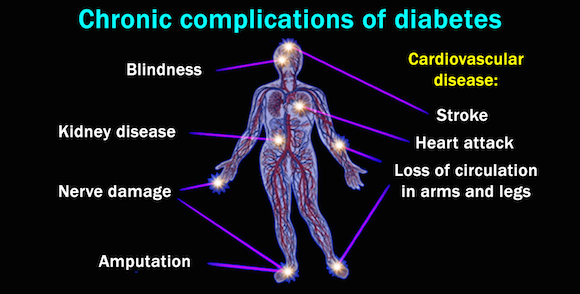
Before insulin was discovered there wasn’t much to effectively treat diabetes. Having too much sugar in the blood is like having poison causing damage to your nerves, blood vessels and organs. Before insulin, most patients with diabetes suffered complications such as blindness, terrible nerve pain, loss of limbs, kidney failure and heart attacks, and died within a few years of being diagnosed.
Today the story is much different because we can do something about it. We know that, for most patients, keeping the A1c less than 7 and keeping the blood sugar levels between 80-130 mg/dL before meals and less than 180 mg/dL 2 hours after meals is the best way to avoid the complications that happen when the sugar rises and is left untreated. This is why diabetics’ “goals of therapy” are so important to establish and frequently review with their health care provider or pharmacist.
I once heard a diabetic educator refer to diabetes as “sugar coated heart disease” and that description really stuck with me. At the end of the day, controlling your blood sugar means protecting your heart and other organs. It is extremely scary to allow blood sugar to run a little high all the time. There may be no alerting signs or symptoms, and it’s easy to think nothing really bad is happening.
In reality, that’s when the most severe damage is occurring. In fact, daily sugars in the low 200s is a big deal and in reality is like having a little bit of poison flowing through vessels every day causing tiny amounts of damage until finally one day, vision starts to go, kidneys stop working, hands and feet are in constant pain and no medication will make the pain stop.
If you have diabetes, don’t let that be you! Start today. Talk to your doctor about your diabetes and come up with a care plan. Know what your goals are for your blood sugar, A1c, blood pressure, and cholesterol.
Understand and Take Advantage Of Available Resources
Diabetes control is an art that sometimes takes time before you get it just right, which is why it’s important to start now and don’t give up or get frustrated if everything doesn’t fall into place right away.

Being a pharmacist myself, I’m often surprised when patients tell me they didn’t realize they could get help with their diabetes control from their pharmacist. Whether it’s the pharmacist that fills your medications or the one that works for your insurance provider, we can help guide patients through the process and answer any questions about medications, insulin administration and blood sugar monitoring.
If you have Medicare insurance, ask your insurance provider about the services that are covered under your part B plan. These usually include testing supplies as well as diabetes self-management classes and more. Even if you’ve had a rough time controlling your diabetes in the past, it’s never too late to start getting serious about keeping your sugar under control.
ABOUT THE AUTHOR

Myla Ross is a Resident Pharmacist at Health First Health Plans, Inc. in Rockledge. She will be completing her one-year post graduate residency in managed care and ambulatory care with the health plans in June 2017. She was born and raised in Melbourne and lives there now with her fiancée, who is also a Pharmacist and works for Publix. Her interests include formulary management and direct patient care.
















