Is There A Doctor In The House?
By Kelley Dunn, Senior Director with Merritt Hawkins // May 10, 2012
Healthcare Dynamics
VIDEO: FOX NEWS
EDITOR’S NOTE—Even though the constitutionality and fate of the Patient Protection and Affordable Care Act (PPACA) presently sit in the capable hands of the U.S. Supreme Court with a judgement due in June, and no matter what the justices decide, the costs of supplying insurance to protect a broader scope of our population will undoubtedly continue to be a socioeconomic-political football and be debated for years to come. However, one very fundamental truth, which raises a major question remains. There will be an increased demand for primary care physicians (PCP), but where will this new wave of PCPs come from and–bottom line–who will see all of the new patients?
There is a looming crisis in primary care, with the shortfall of doctors estimated at 30,000 over the next couple of years. An aging PCP physician population and increasing elderly population certainly contribute to the problem. However, a proclivity of new physicians for “hospital medicine,” such as emergency medicine physician and hospitalists, physicians who take care of hospitalized patients but no longer have office-based practices or do primary care, has also taken thousands of physicians out of the potential primary care workforce.
The student debt incurred during the long and costly training cycle also drives young physicians away from the rapidly depleting ranks of primary care to more lucrative specialty medicine and surgery careers.
SpaceCoastDaily.com is delighted to welcome Kelley Dunn, Senior Director with Merritt Hawkins, one of the leading physician search and consulting firms in the U.S., to share the results of her research regarding the impending physician shortage with SpaceCoast Daily.com.
The Physician Shortage By The Numbers
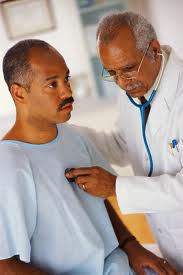
Is there a doctor in the house?
That question, long a staple of old school comedy routines, is no longer one that can be taken lightly. For a variety of reasons, demand for physicians in Florida and throughout the United States is outpacing supply. A quarter of Florida’s practicing physicians are over 65. These statistics will only increase the demand for physician services in the future for Florida’s population, which is projected to increase 60% by 2030. Florida’s aged population is projected to grow by 124% during the same time frame.
Without going into too much detail, the shortage is largely a result of two divergent trends. On the one hand, the number of physicians trained in the United States has remained flat for about the last 25 years. On the other, the population has grown significantly and has become older, requiring more physician services.
The physician shortage is likely to be exacerbated by health reform, which may add over 30 million people to the ranks of the insured, driving demand for physicians even higher.
The way physicians practice also is a factor. A growing number of doctors are choosing to select specialties that afford shift work with no call responsibility, work part-time, or on a temporary basis, diminishing the ready supply of active primary care physicians.
The following facts and trends underline the seriousness of today’s growing physician shortage.
- The Association of American Medical Colleges (AAMC) forecasts that in 15 years the United States will face a deficit of up to 159,300 physicians. The AAMC projects that universal access to health care would increase the physician shortage by an additional 31,000 doctors. The AAMC has consequently called for a 30% increase in the number of physicians trained in the U.S.
- The American Academy of Family Physicians (AAFP) projects a shortage of 149,000 physicians by 2020, while the Health Resources and Services Administration (HRSA) projects a shortage of 65,560 primary care physicians by 2020.
- Twenty-four states have released reports projecting physician shortages, and 21 medical specialty societies have released reports projecting shortages in their fields.
- Between 1987 and 2007 the population of the United States grew 24 percent, from 242 million people to 302 million people. In the same period, the number of physicians trained in the U.S. grew by only 8%.
- In addition to an emerging physician shortage, there is a long-standing maldistribution of physicians in the United States (CLICK HERE to view an interactive national map showing the relative availability of primary health care providers by county) with fewer doctors practicing in rural and inner city areas.
- The Health Services and Resources Administration (HRSA) currently designates over 6,200 Health Professional Shortage Areas (HPSAs) for primary care nationwide, in which over 65 million people live. Sixty-seven percent of HPSAs are in non-urban areas. The ratio of primary care providers to patients in these areas is less than one per 2,000.
- HRSA projects it would take 17,000 additional primary care clinicians to achieve a ratio of one primary care giver per 2,000 patients in the nation’s 6,200-plus HPSAs.
- HRSA also currently designates 3,291 mental health HPSAs nationwide in which 80 million Americans live.
- While some 20 percent of Americans live in rural areas, only nine percent of physicians practice in rural areas.
- Fewer than one percent of final-year medical residents would prefer to practice in communities of 10,000 people or less.
- Between 2002 and 2007, the number of U.S. medical school graduates choosing to become family physicians decreased by 25 percent. Adding to the looming shortage of PCPs is the fact that hospital medicine is the fastest growing specialty in American medical history, and according to statistics compiled by the Society of Hospital Medicine (SHM), the number of doctors practicing as hospitalists has increased 172 percent from 2003 to 2010.
- Forty-two percent of patient visits to the doctor in rural areas are seen by family physicians, compared to 23 percent for all Americans.
Like many other challenges in health care today, solving the physician shortage will not be easy. The physician training cycle is a long and costly one, and even if the resources were committed today to train more doctors, it would take years before this would have a significant effect on physician supply.
In the interim, physicians will need to rethink how they practice, doing what they can to delegate responsibilities to other clinicians when appropriate. Patients can expect longer appointment wait times and more difficulty in finding physicians who can address their individual needs.
Yes, there will be a doctor in the house, but in the coming years, he or she will be increasingly hard to find.
ABOUT THE AUTHOR
 Kelley Dunn is Senior Director with Merritt Hawkins, the leading physician search and consulting firm in the United States and a company of AMN Healthcare (NYSE: AHS). She earned a double major in Biology and Chemistry from the University of Georgia, a Masters degree from Florida Atlantic University, and is currently a faculty instructor with the University of Florida. With over 8 years of healthcare staffing experience, Kelley has consulted with over 2,000 clinics and hospitals in Florida.
Kelley Dunn is Senior Director with Merritt Hawkins, the leading physician search and consulting firm in the United States and a company of AMN Healthcare (NYSE: AHS). She earned a double major in Biology and Chemistry from the University of Georgia, a Masters degree from Florida Atlantic University, and is currently a faculty instructor with the University of Florida. With over 8 years of healthcare staffing experience, Kelley has consulted with over 2,000 clinics and hospitals in Florida.
She can be reached at Kelley.dunn@merritthawkins.com













1 Trackback / Pingback