HEALTH SPOTLIGHT: Antibiotic Allergies in Children, Are We Mislabeling Many of Them?
By Christopher Johnson, MD // May 2, 2018
assessing possible antibiotic allergies

EDITOR’S NOTE: Space Coast Daily is delighted to welcome Dr. Christopher Johnson as a guest contributor on issues of child health and well-being. With 35 years of experience practicing pediatrics, pediatric critical care (intensive care), and pediatric emergency room care he is committed to educating parents on how best to meet the needs of the ill and injured child in today’s often confusing and complex healthcare system.
In this article, Dr. Johnson provides sage insight into and advice related to assessing possible antibiotic allergies, and how they are probably grossly overestimated.
— Dr. Jim Palermo, Editor-in-Chief
Around 10% of children in America are labeled as allergic to penicillin or a member of the penicillin family of antibiotics. Besides penicillin, children are often labeled allergic to other commonly used antibiotics. Is this even close to correct?
The answer is probably not. We now understand that most of the cutaneous symptoms that are interpreted as drug allergy are likely viral induced or due to a drug–virus interaction, and they usually do not represent a long-lasting, drug-specific, adaptive allergic immune response to the antibiotic that a child received.
This observation points out that many oral antibiotics are prescribed, inappropriately, for viral illnesses, typically respiratory infections. It’s a problem because most of the time these children carry the allergic label into adulthood.
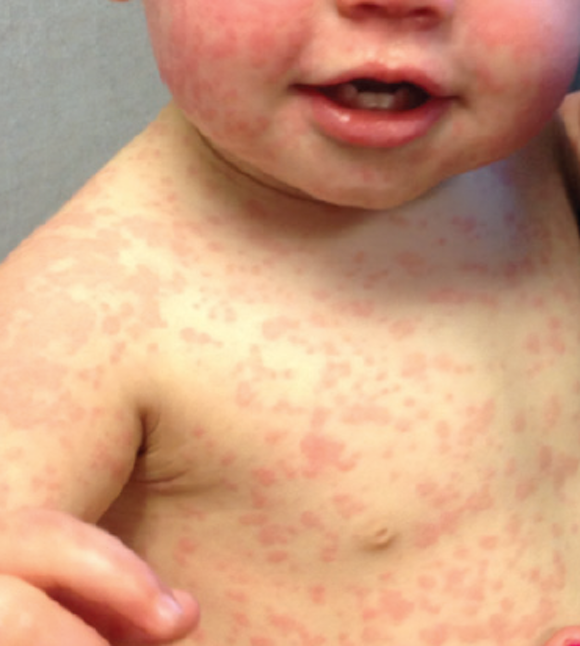
A very common example is the drug amoxicillin, which is a cousin to ampicillin, members of the penicillin family. It’s been known for a long time that a rash with ampicillin or amoxicillin is common and usually doesn’t signify a true allergy. But it might. I and many of my colleagues write in the child’s medical record “rash with ampicillin” as an addendum to the “penicillin allergic” notation. This tells the next physician that the allergy may very well be real. A recent review examines the implications of this problem.
In practice, we often avoid the issue by choosing another antibiotic than the one the child is labeled allergic to, but sometimes this means selecting less than the best medication or, as many parents can attest, a much more expensive one. It also can mean using an antibiotic that is best saved for more severe and unusual infections. When we overuse an antibiotic, bacteria often develop resistance to it, eliminating it from our arsenal for the future.
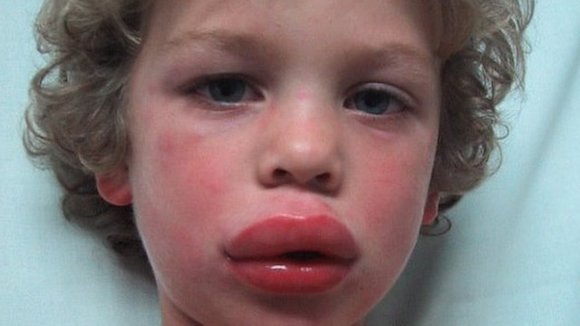
There is one rash — hives — that is characteristic of true allergy. This can be accompanied by wheezing or facial swelling. If your child experienced that after receiving an antibiotic then it’s likely to be a true allergy. This is why a good physician will inquire what the alleged allergy symptoms were before deciding.
For example, I’ve had parents who were told, or decided themselves, their child was allergic because of very vague and clearly non-allergic symptoms, such as abdominal pain, fatigue, or behavioral changes. Some antibiotics do indeed upset the stomach, but that’s not an allergy. A better term is drug intolerance.
If it’s important to know if your child is truly allergic, there are tests we can do to make sure. These can include skin testing or a medically supervised small test dose. The authors of the review recommend physicians do more of these, rather than just allowing the allergic label to persist in the minds of the parents and in the medical record.
ABOUT THE AUTHOR

Dr. Christopher Johnson received his undergraduate education in history and religion at Haverford College in Haverford, Pennsylvania, where he graduated magna cum laude in 1974. He earned his Doctor of Medicine degree in 1978 from Mayo Medical School in Rochester, Minnesota, then trained in general pediatrics at Vanderbilt University Children’s Hospital in Nashville, Tennessee, followed by training in pediatric infectious diseases, hematology research, and pediatric critical care medicine at the Mayo Graduate School of Medicine. Dr. Johnson is certified by the American Board of Pediatrics in general pediatrics and in pediatric critical care medicine and is a Fellow of the American Academy of Pediatrics.
Dr. Johnson, who has been named to a list of “The 50 Best Mayo Clinic Doctors — Ever,” devotes his time to practicing pediatric critical care as President of Pediatric Intensive Care Associates, P.C., as Medical Director of the PICU for CentraCare Health Systems, and to writing about medicine for general readers. His popular website/blog and four books provide a wealth of information and answers to practical questions related to child health issues.
CLICK HERE FOR BREVARD COUNTY NEWS














